If You Want a Better World, Become a Quantum Activist
December 26, 2019
The Freedom Checklist – What Every Human Being Needs to Know
December 5, 2021
Scorpio Full Pink Moon – Deep Dive Video inc All Signs…
April 22, 2024
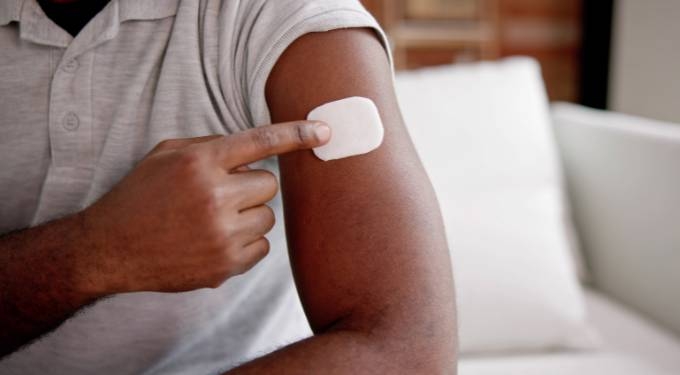
Do Vaccines Make Us Healthier? (2024 update)
April 21, 2024
Weekly Astrology Video WC 22nd April 2024 + All Signs
April 21, 2024
German Government Admits There Was No Pandemic
April 15, 2024
Paralyzed Woman's Bond With Her Horse Transforms Her Life
April 15, 2024

















![A Higher Energy Is Trying To Do Something – Kyle Cease [Video]](https://consciouslifenews.com/wp-content/uploads/2024/04/kyle-cease-its-not-working-350x250.jpg)